Frozen Shoulder: Symptoms, Stages and Treatments
By: Dr. Daniel Welch, DC
As a chiropractor that focuses on sports injury cases, shoulder injuries present regularly to the clinic. Determining a differential diagnosis is one of the first things we are trained to do. Shoulder pain is easy to diagnose when a history reveals a recent traumatic injury to the joint, but pain can originate from other areas as well. Many patients have referred pain from the neck, rotator cuff injuries, labral tears, and even occasionally non-musculoskeletal complaints such as pulmonary or cardiac derived pain. Diagnosis is very important to determine an appropriate treatment plan.
One ailment that I find interesting is adhesive capsulitis commonly referred to as frozen shoulder. This complaint presents as stiffening of the shoulder joint, causing immobility and pain.
Adhesive capsulitis (frozen shoulder) is typically categorized in four stages:
- The Prefreezing Phase is noted as the start of frozen shoulder. It is difficult to determine what is wrong with the shoulder in this phase, with non-specific pain, even at rest. The pain will be present as a dull ache without movement, transitioning to sharp pain with movement. Over head reach and external rotation will be most provocative, causing hesitancy in motion. Pain and stiffness will be slowly progressing for 1-3 months in this phase.
- The Freezing Phase is more an extension of the first stage. Symptoms can continue to increase for nine months. Shoulder range of motion and pain will progress (especially at night). Motion will still exist, but with increasing sharp pain. This is the stage where patient’s are typically presenting to the clinic after over the counter medications is not addressing the symptoms.
- The Frozen Stage is characterized with very limited mobility and pain with initiating motion. This can vary patient to patient, but commonly presents one year from onset of pain. Patients typically report that pain will start to reduce before mobility returns.
- The Thawing Stage (and the last stage) consists of significant reduction in shoulder pain, and slow but steady improvement in range of motion. Overhead reach is usually the last range to return due to the complex nature of the movement necessitating scapular and clavicular (collar bone) coordination. Patient’s can sleep better at this phase and have improved reported outlook since they are nearing pre-injury status. There are multiple factors that can alter the length of this phase, but periods of 12-15 months are common.
What Causes Frozen Shoulder?
The cause of this ailment is up for debate. The most common theory is that inflammation of the synovial tissue (lining of the joint space) causes an auto-immune reactions involving the body attacking its own tissue. The shoulder is a joint that is used constantly throughout the day. It is a complicated joint that relies on a series of tendons, ligaments, and three bones to function. The joint is encased in a connective tissue capsule. Overtime, with improper alignment, the joint is not always positioned properly, allowing for wear and tear to cause micro tears to the capsule, resulting in swelling. This swelling can lead to scarring of the capsule, initiating the immobility and pain. Other risk factors include:
- Pre-existing diabetes diagnosis or hyperthyroidism
- Immobility after a surgery or stroke
- Pain from a degenerative joint, impingement, or tendinosis resulting in a hesitancy of moving the joint
Treatments for Frozen Shoulder
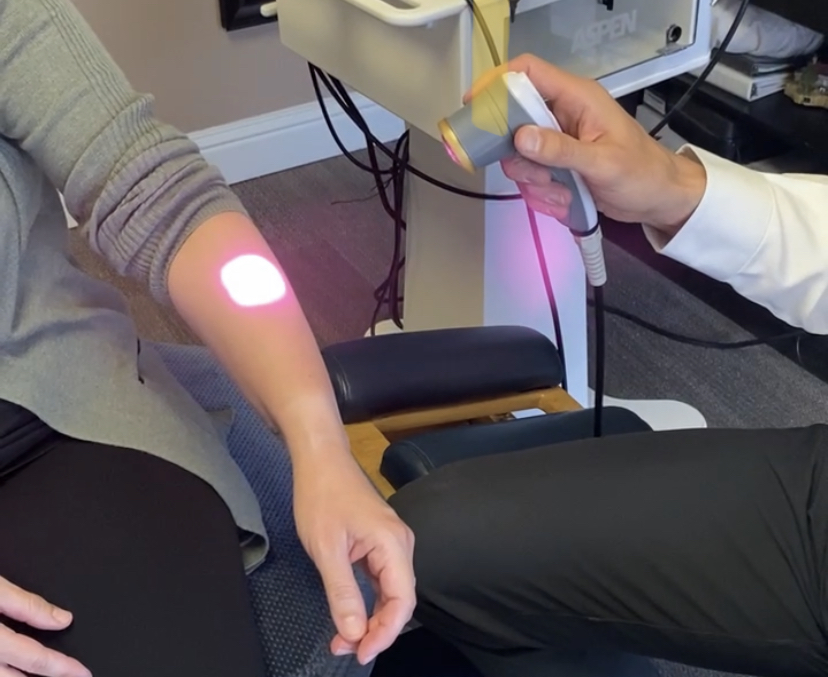
Treatment of Adhesive capsulitis involves initially pain modulation protocols and therapies to restore mobility. At first, patients are not inclined to actively use the shoulder, so light passive (assisted) range of motion (ROM) protocols are utilized along with certain therapeutic modalities. Goals at this stage are to improve mobility, inch by inch. In our office, manual therapies such as proprioceptive neuromuscular facilitation (PNF), laser therapy, and electric stimulation are used to treat adhesive capsulitis. A recent meta-analysis demonstrated the effectiveness of PNF for decreasing pain, reducing disability, and increasing ROM. (1)
As symptoms start to improve, techniques such as active release, manipulation and active rehab protocols are used. Interestingly, although ultrasound has been used for years as a common treatment protocol, ultrasound added in combination to physical therapy modalities did not provide any additional benefits for the treatment of adhesive capsulitis according to recent study. (2)
If conservative therapies are not effective, additional therapies may be referred out for. These include, but are not limited to:
- Corticosteroid injections
- Manipulation under anesthesia
- Hyaluronic acid injection
- Capsular release surgery
- Extracorporeal shock wave therapy
With this stated, the vast majority of adhesive capsulitis cases do not involve surgery/invasive treatments. Although this is a typically slow ailment to heal from, full recovery is possible. There is a chance of developing adhesive capsulitis more than once. This is why it is strongly recommended that patients perform recommended rehab after a frozen shoulder to limit the chance of possible future flare-ups.
If you have any questions about adhesive capsulitis, or are interested in a consultation, feel free to contact our office.
1. (Tedla and Sangadala, 2019) Proprioceptive neuromuscular facilitation techniques in adhesive capsulitis: a systemic review and meta-analysis
2. (Balki et al., 2018) Efficacy of therapeutic ultrasound in treatment of adhesive capsulitis: A prospective double blind placebo-controlled randomized trial